
Research and studies have explored how obesity causes erectile dysfunction. Several studies indicate that obesity increases the risk of developing erectile dysfunction due to its negative impact on vascular health and hormone levels. The accumulation of abdominal fat, often associated with obesity, has been linked to impaired blood flow to the pelvic region, leading to erectile problems. Understanding the connection between obesity and erectile dysfunction is essential in developing effective prevention and treatment strategies to address this significant health concern. We will discuss pretty much all aspects of obesity and provide appropriate ways you can use for your well-being.

For example, “behavioral therapy for obesity” is an approach that is not often portrayed as it should be in weight-loss programs.
There are a few programs that cover most if not all of the needs of affected people, such as Noom. [Important note: We are not an affiliate partner of NOOM. We present NOOM only because many people have benefitted of their weight loss program.]
Noom is a lifestyle-focused mobile app that can be easily downloaded to your smartphone or tablet. With its emphasis on behavioral changes rather than a restrictive diet, Noom offers a unique approach to achieving a healthier lifestyle.
The app provides a range of features and resources to support your journey, including:
- Weekly challenges and educational content: Gain valuable insights on nutrition, stress management, goal setting, and forming healthy habits through engaging weekly challenges and informative materials.
- Progress tracking tools: Keep track of your meals, exercise routine, and body weight using Noom’s intuitive tracking tools. This allows you to monitor your progress and make informed decisions about your health.
- Virtual coaching team and Noom Circles: Access a supportive network of health coaches and join interest-based communities called Noom Circles. These resources are designed to provide guidance, motivation, and accountability throughout your journey.
- Biometric tracking capabilities: Utilize Noom’s biometric tracking features to monitor essential health indicators such as blood sugar and blood pressure levels. This empowers you to stay informed about your health and make necessary adjustments.
If you’re intrigued by Noom but still unsure, you can take advantage of their 7-day trial to explore the app’s features and determine if it’s the right fit for you.
This trial period allows you to experience Noom firsthand before committing to the monthly fee.
Read the entire article to get informed on almost all the most up-to-date information on causes, methods of prevention and treatment, be it invasive or non-invasive, and alternative treatments for obesity backed by scientific studies.
At the very end, we have provided 10 studies on 10 different natural supplements that may help with obesity.
But let’s clarify how obesity is related to erectile dysfunction. Below are some facts that have been summarized from scientific studies.
Does Obesity Cause Low Testosterone?
Obesity can have an impact on men’s hormone levels, particularly their total and free testosterone levels, which tend to be lower in obese men.
Testosterone is a vital hormone for males and is responsible for several characteristics such as a deep voice, the development of male sexual organs, large muscles, and strong bones.
Additionally, testosterone plays a crucial role in sperm production and libido in men.
Another important aspect of testosterone is its conversion to dihydrotestosterone, which helps in the growth of the prostate. The hormone’s production begins to increase during puberty and reaches its peak in early adulthood, after which it tends to plateau and then gradually decline with age.
But by the way, nowadays there are many methods to treat erectile dysfunction.
BMI Increase – Waist Size & Erectile Dysfunction
Studies have shown that for men over the age of 40, every one-point increase in their body mass index (BMI) results in a 2% decrease in testosterone levels.
Additionally, for men aged 30 years and above, a four-inch increase in waist size increased their risk of having low testosterone levels by 75%.

According to an Australian study, one out of every seven obese men could benefit from testosterone replacement therapy.
This rate is more than four times higher than the corresponding rate in men of normal weight.
Testosterone replacement therapy can help increase testosterone levels in men, improving their overall health and well-being.
Although hormonal disorders and low testosterone levels account for only 3% of cases of erectile dysfunction, obese men still face an increased risk of developing the condition, even with normal testosterone levels.
Research has found a strong correlation between abdominal obesity and erectile dysfunction, particularly in older men.
According to these studies, men with a BMI of 28 have a 90% increased risk of developing erectile dysfunction.
Excessive heat in the testes has been found to be associated with low sperm count.
Specifically, excess fat in the pubic region and inner thighs can cause the testes to reach temperatures over 35˚C, which may be sufficient to hinder sperm production.
However, there is hope for obese men experiencing erectile dysfunction. Losing weight has been linked to a significant improvement in symptoms.
In addition to increasing the risk of erectile dysfunction, obesity in men is also associated with a lower frequency of sexual intercourse.
A BMI Of 25 Or Higher – The link Between Obesity & Prostate Problems
Obesity has been found to be associated with a benign enlargement of the prostate that is common in older men. Specifically, men with waist sizes of 43 inches or larger are 2.4 times more likely to require surgery for Benign Prostate Hyperplasia than those with waists smaller than 35 inches.

The prostate gland releases a protein called Prostate-Specific Antigen (PSA), and as the gland enlarges, the PSA levels rise.
However, obesity has been shown to lower PSA levels. Research has found that in Caucasian men aged 40 and over, each five-inch increase in waist circumference leads to a 6.6% decrease in blood PSA levels.
This decrease may not be due to low PSA production but rather due to dilution of blood in obese individuals.
PSA is an important indicator of the progression of prostate cancer. Studies have also linked excess body fat to an increased risk of developing prostate cancer.
According to the American Cancer Society, being overweight increases a man’s risk of prostate cancer by 8%, while obesity raises the risk by 20%, and severe obesity increases the risk by 34%.
In addition, obesity can cause the recurrence of prostate cancer and increase the risk of its spread to other organs. [ncbi.nlm.nih.gov]
Obesity & Erectile Dysfunction – Common Solution
Obesity and erectile dysfunction (ED) often have similar metabolic problems, like insulin and leptin resistance, which contribute to ED.
Below is the summary of a scientific study [Obesity and Erectile Dysfunction: From Bench to Clinical Implication]:
(Metformin, a drug originally used for diabetes, can reduce these issues. It helps by sensitizing insulin and reducing leptin resistance.
Metformin has shown potential in normalizing the underlying problems associated with obesity and increasing the effectiveness of ED treatment with drugs called phosphodiesterase 5 inhibitors (PDE5 inhibitors).
Combining metformin with PDE5 inhibitors may be an effective method for treating ED in individuals with obesity.
Metformin, a medication used to treat diabetes, has shown to have effects in reducing erectile dysfunction (ED).
It has anti-inflammatory and anti-obesity properties. Metformin affects blood vessels, even when there is no significant impact on blood sugar control.
It activates a molecule called AMPK, which plays a role in regulating energy levels in cells.
The exact mechanism of how metformin works is not fully understood, but it has been shown to have various beneficial effects on the lining of blood vessels, including activating NOS (a molecule involved in blood flow), reducing oxidative stress, increasing the breakdown of fatty acids, and reducing stress in cells.
It means that Metformin enhances the ability of blood vessels to widen in patients with metabolic syndrome.
Combining metformin with testosterone treatment has also been found to increase erectile function in individuals with obesity and low testosterone levels.
Phosphodiesterase 5 inhibitors (PDE5 inhibitors) are commonly prescribed to treat erectile dysfunction (ED).
Besides their direct effects on ED, PDE5 inhibitors have been linked to improved insulin sensitivity, which is important for managing diabetes.
Some specific PDE5 inhibitors, such as sildenafil and udenafil, have been associated with weight loss effects and reduced visceral fat in obese individuals.
Additionally, PDE5 inhibitors have been found to lower the risk of overall mortality in patients with type 2 diabetes.
Combining phosphodiesterase 5 inhibitors (PDE5 inhibitors) with metformin could be a more effective way to treat erectile dysfunction (ED) in patients with obesity and other medical conditions.
The combination of metformin and PDE5 inhibitors has been found to be effectiv for individuals with insulin resistance and obesity-related ED.)
The Link Between Obesity And Erectile Dysfunction In Summary
- Obesity can restrict blood flow to the penis and make it difficult to achieve or maintain an erection.
- It can lead to a decrease in testosterone levels, which can result in low libido and erectile dysfunction.
- It can cause psychological distress, including depression, anxiety, and low self-esteem, which can affect sexual desire, arousal, and strength.
- Certain medications used to treat obesity, such as antidepressants and antihypertensive drugs, can also cause sexual dysfunction.
- Sleep apnea, a condition in which a person’s breathing is interrupted during sleep, is commonly associated with obesity and has been linked to erectile dysfunction and decreased libido in men.
- Obesity is associated with chronic low-grade inflammation, which can lead to damage to blood vessels and nerves that affect sexual function.
- It is often accompanied by other health conditions, such as high blood pressure, high cholesterol, and insulin resistance, which are collectively known as metabolic syndrome. Metabolic syndrome can also contribute to sexual dysfunction.
Penile Traction Devices For ED & Low Testosterone
-
We provided in our article on penile traction devices and vacuum pumps 20 scientific studies showing the effects of these devices. They are used as a treatment for erectile dysfunction. There are studies proving their effectiveness in increasing penis sensitivity and erectile strength but their effectiveness in obese individuals specifically has not been extensively studied.
- These devices work by applying a constant gentle force to the penis over a prolonged period of time, with the goal of stretching the penile tissue and increasing blood flow to the penis.
- Obesity can contribute to erectile dysfunction by restricting blood flow to the penis and causing damage to blood vessels and nerves that affect sexual function.
- Penile traction devices may be able to help improve erectile function in obese individuals by increasing blood flow to the penis and promoting tissue growth.
- However, obesity can also affect hormone levels, particularly testosterone, which is essential for sexual function. Penile traction devices are unlikely to address hormonal imbalances and may not be effective in improving erectile function in individuals with low testosterone levels.
- The use of penile traction devices as a treatment for erectile dysfunction in obese individuals is an area that requires more research.Obesity is a medical condition characterized by excess body fat that increases the risk of health problems. It is defined as having a body mass index (BMI) of 30 or higher. BMI is calculated by dividing a person’s weight in kilograms by their height in meters squared.Itcan lead to various health problems, such as type 2 diabetes, high blood pressure, heart disease, stroke, and certain types of cancer.It can also affect a person’s quality of life, as it can limit mobility, lead to low self-esteem, and cause social discrimination.Obesity is often caused by a combination of genetic, environmental, and lifestyle factors, such as overeating, lack of physical activity, and hormonal imbalances.Treatment typically involves a combination of diet and exercise, as well as behavioral and psychological support.
In some cases, medications or surgery may be recommended.
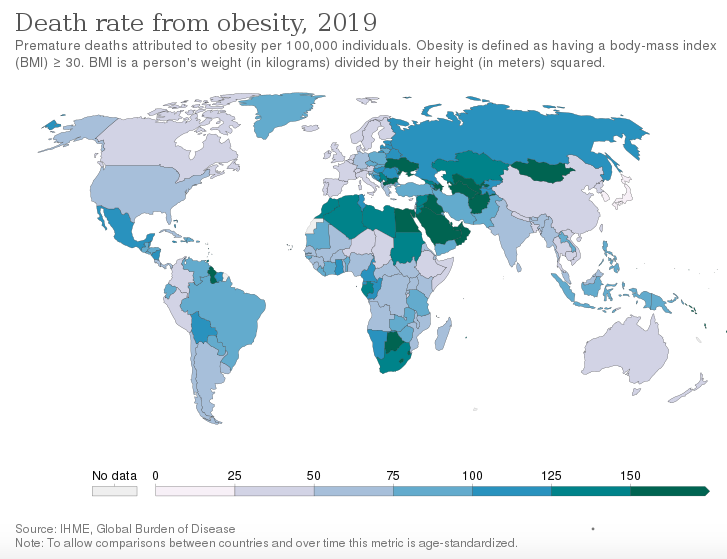
https://ourworldindata.org/grapher/death-rate-from-obesity
Types Of Obesity
There are generally two types of obesity:
- Android obesity: This type of obesity is characterized by the accumulation of excess body fat in the abdominal area, resulting in an apple-shaped body. People with android obesity are more likely to develop health problems such as type 2 diabetes, high blood pressure, and heart disease. This type of obesity is more common in men than in women.
- Gynoid obesity: This type of obesity is characterized by the accumulation of excess body fat in the hip and thigh area, resulting in a pear-shaped body. People with gynoid obesity are less likely to develop health problems than those with android obesity. This type of obesity is more common in women than in men.
What Are The Causes Of Obesity?
There are many different factors that can contribute to the development of obesity, including:
- Genetics: Some people may have a genetic predisposition to obesity, meaning they are more likely to gain weight and store fat.
- Environmental factors: The availability of high-calorie, low-nutrient foods and the prevalence of sedentary lifestyles can contribute to weight gain.
- Lifestyle factors: Poor dietary choices, such as a diet high in processed foods, and lack of physical activity can lead to weight gain.
- Medical conditions: Certain medical conditions, such as hypothyroidism, Cushing’s syndrome, and polycystic ovary syndrome (PCOS), can contribute to weight gain.
- Medications: Some medications, such as antidepressants, antipsychotics, and corticosteroids, can cause weight gain as a side effect.
- Psychological factors: Emotional eating, stress, and other psychological factors can contribute to overeating and weight gain.
It’s important to note that obesity is often caused by a combination of these factors, and that each individual’s situation is unique. Effective treatment typically involves a personalized approach that addresses the underlying causes of the condition.
What Is The Prevalence Of Obesity?
The prevalence of obesity has been increasing globally in recent years.
According to the World Health Organization (WHO), in 2016, more than 1.9 billion adults were overweight, and of these, over 650 million were obese.
In the United States, the prevalence of obesity is particularly high. The current prevalence of obesity in USA is nearly 34% of the population is overweight or obese, which corresponds to about 103 million people in 2021.
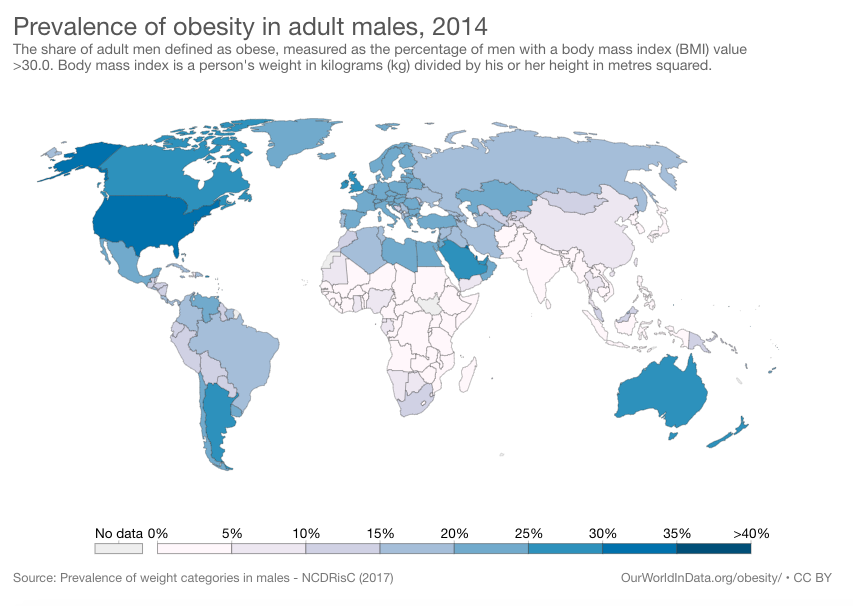
[Source: Our World In Data, CC BY 3.0 <https://creativecommons.org/
According to the Centers for Disease Control and Prevention (CDC), in 2020, the obesity prevalence was 42.4% among adults in the US, with a BMI of 30 or higher.
This means that nearly half of all adults in the US are considered obese.
The prevalence of obesity is also high among children and adolescents in the US, with approximately 19% of children and 20% of adolescents being classified as obese.
Obesity is a major public health concern because it increases the risk of numerous health problems, including heart disease, stroke, diabetes, and certain types of cancer.
Reducing the prevalence of obesity is therefore an important public health priority.
Best Conventional Treatments & Prevention Of Obesity
There are several different treatments available for obesity, and the most effective approach typically involves a combination of different strategies. Some of the most common treatments for obesity include:
[by Nick Youngson CC BY-SA 3.0 Pix4free.org]
- Dietary changes: Reducing calorie intake and making healthier food choices can help individuals lose weight.
- Physical activity: Regular exercise can help individuals lose weight and improve overall health.
- Behavioral therapy: Behavioral therapy can help individuals develop healthier habits and coping strategies to manage food cravings and emotional eating.
- Medications: Certain medications, such as appetite suppressants and medications that reduce the absorption of fat, may be prescribed to help individuals lose weight.
- Bariatric surgery: For individuals with severe obesity, bariatric surgery may be recommended. This involves surgical procedures that reduce the size of the stomach, limiting the amount of food that can be consumed.
It’s important to note that there is no one-size-fits-all approach to treating obesity, and the most effective treatment plan will depend on an individual’s unique circumstances and medical history.
Working with a healthcare provider or registered dietitian can help individuals develop a personalized plan for managing obesity and improving overall health.
Managing Obesity: A Holistic Approach Backed by the Endocrine Society
Obesity is a complex condition that requires a multifaceted approach for effective management. The Endocrine Society, a leading authority in the field, emphasizes the importance of incorporating diet, exercise, and behavioral modifications as the foundation of all obesity management strategies.
In addition to these lifestyle changes, there are other tools available, such as weight loss medications and bariatric surgery, which can be combined with behavioral adjustments to further support individuals in their weight loss journey.
Let’s delve into the key recommendations put forth by the Endocrine Society.
- Incorporate Lifestyle Changes: The Endocrine Society strongly advocates for the inclusion of diet, exercise, and behavioral modifications as the primary components of any obesity management plan. By making sustainable changes to dietary habits, engaging in regular physical activity, and adopting healthy behaviors, individuals can effectively reduce their food intake and increase their overall level of physical activity.
- Weight Loss Medications: In cases where lifestyle changes alone may not yield the desired outcomes, weight loss medications can be considered as a complementary tool. If a patient responds positively to a weight loss medication and loses 5 percent or more of their body weight within three months, it is recommended to continue the medication. However, if the medication proves ineffective or causes adverse side effects, it should be discontinued, and alternative medications or approaches should be explored.
- Medications for Diabetes Management: People with diabetes who are overweight or obese should be prescribed medications that either promote weight loss or have no effect on weight gain as first- and second-line treatments. Some diabetes medications are associated with weight gain, which can exacerbate the challenges faced by individuals struggling with obesity. Healthcare professionals should discuss the potential effects of medications on weight with their patients, ensuring informed decision-making regarding treatment options.
- Hypertension Treatment for Obese Individuals with Type 2 Diabetes: Certain types of medication, namely angiotensin converting enzyme inhibitors, angiotensin receptor blockers, and calcium channel blockers, are recommended as first-line treatments for high blood pressure in individuals with Type 2 diabetes who are obese. These medications have been proven effective in managing blood pressure and are less likely to contribute to weight gain compared to alternative medications like beta-adrenergic blockers.
- Weight-Related Effects of Medications: When patients require medications that can potentially impact weight, such as antidepressants, antipsychotic drugs, or epilepsy treatments, it is crucial for healthcare professionals to provide comprehensive information. Patients should be fully informed about the potential effects of each medication on weight, allowing them to make well-informed decisions. The healthcare provider and patient should engage in shared decision-making, thoroughly evaluating the available options based on individual circumstances and goals.
- Considerations and Exceptions: In patients with uncontrolled high blood pressure or a history of heart disease, medications such as phentermine and diethylpropion should be avoided due to associated risks. It is important for healthcare providers to carefully assess each patient’s medical history and tailor the treatment plan accordingly, prioritizing safety and overall well-being.
Conclusion: The Endocrine Society’s recommendations emphasize the importance of a comprehensive and patient-centered approach to obesity management.
By combining lifestyle changes, weight loss medications, and other medical interventions, healthcare providers can provide effective and personalized care.
It is crucial for individuals struggling with obesity to consult with healthcare professionals to explore the most suitable options, taking into account their unique circumstances, preferences, and goals.
Best Methods To Prevent Obesity
Preventing obesity involves making healthy lifestyle choices to maintain a healthy weight. Some effective methods to prevent obesity include:
- Healthy diet: Eating a balanced diet that includes plenty of fruits, vegetables, whole grains, and lean protein can help prevent obesity.
- Regular physical activity: Regular exercise is important for maintaining a healthy weight and overall health. The CDC recommends that adults get at least 150 minutes of moderate-intensity aerobic exercise per week.
- Portion control: Paying attention to portion sizes and avoiding overeating can also help.
Limiting sugary drinks and snacks: Such drinks and snacks are high in calories and can contribute to unexpected and excessive weight gain. - Getting enough sleep: Lack of sleep can disrupt hormones that regulate appetite and can lead to uncontrolled appetite.
- Managing stress: Stress can lead to overeating and weight gain, so managing stress can be helpful. Avoiding smoking and excessive alcohol consumption: Both smoking and excessive alcohol consumption have been linked to weight gain and obesity.
FDA – Approved Medications To Treat Obesity
The U.S. Food and Drug Administration (FDA) has approved several medications for the treatment of obesity.
These medications are intended for use as part of a comprehensive weight loss program that includes dietary changes and increased physical activity.
Here are some FDA-approved medications for obesity:
- Orlistat: Orlistat (brand name Xenical) is a lipase inhibitor that works by blocking the absorption of dietary fat. It is approved for use in adults with a BMI of 30 or higher, or a BMI of 27 or higher with an obesity-related health condition such as high blood pressure or type 2 diabetes. Orlistat is available by prescription and over-the-counter in a lower dose as Alli.
- Phentermine: Phentermine (brand names Adipex-P, Lomaira) is an appetite suppressant that works by reducing hunger and increasing feelings of fullness. It is approved for short-term use in adults with a BMI of 30 or higher, or a BMI of 27 or higher with an obesity-related health condition. Phentermine is available by prescription only.
- Liraglutide: Liraglutide (brand name Saxenda) is a glucagon-like peptide-1 (GLP-1) receptor agonist that works by increasing feelings of fullness and reducing hunger. It is approved for use in adults with a BMI of 30 or higher, or a BMI of 27 or higher with an obesity-related health condition. Liraglutide is available by prescription only.
These medications are not a 100% cure for obesity, and they are not appropriate for everyone. They can have side effects, and they are not suitable for people who are pregnant or have certain medical conditions such as uncontrolled high blood pressure or heart disease.
What Is Bariatric Surgery & How Does It Work
Bariatric surgery is a surgical intervention that is typically reserved for individuals with severe obesity who have not been able to achieve significant weight loss through other methods.
Bariatric surgery can be an effective treatment option for individuals who have a BMI of 40 or higher, or a BMI of 35 or higher with an obesity-related health condition.
There are several types of bariatric surgery, including:
Roux-en-Y gastric bypass: This surgery involves creating a small pouch in the stomach and connecting it to the small intestine, bypassing the rest of the stomach and upper small intestine.
Sleeve gastrectomy: This surgery involves removing a large portion of the stomach, leaving a smaller tube-shaped stomach.
Adjustable gastric banding: This surgery involves placing an inflatable band around the top portion of the stomach, creating a smaller stomach pouch.
Bariatric surgery can lead to significant weight loss and improvements in obesity-related health conditions such as type 2 diabetes, high blood pressure, and sleep apnea.
However, it is important to note that bariatric surgery is a major surgical intervention that carries risks and potential complications.
Scientific Research On Meciations & Bariatric Surgery For Obesity
Both medications and bariatric surgery can be effective in achieving significant weight loss and improving obesity-related health conditions for individuals with obesity.
For medications, research suggests that they can lead to modest weight loss in the short term.
For example, a meta-analysis of 28 randomized controlled trials found that participants taking orlistat lost an average of 2.9 kg (6.4 lbs) more than participants taking a placebo over 1 year.
Similarly, a meta-analysis of 9 randomized controlled trials found that participants taking liraglutide lost an average of 4.4 kg (9.7 lbs) more than participants taking a placebo over 1 year.
For bariatric surgery, research suggests that it can lead to significant and sustained weight loss, as well as improvements in obesity-related health conditions.
For example, a systematic review and meta-analysis of 164 studies found that, on average, individuals who underwent bariatric surgery lost about 26 kg (57.3 lbs) and experienced significant improvements in type 2 diabetes, high blood pressure, and sleep apnea.
More Scientific Studies On The Success Rate Of Bariatric Surgery
There are many studies available on the effectiveness of bariatric surgery for treating obesity. Here are some examples:
- A systematic review and meta-analysis published in Obesity Surgery in 2020 found that, on average, individuals who underwent bariatric surgery lost about 25 kg (55 lbs) and experienced significant improvements in type 2 diabetes, high blood pressure, and sleep apnea.
- A study published in JAMA Surgery in 2020 found that 5 years after bariatric surgery, nearly 70% of individuals achieved a weight loss of 20% or more and nearly 85% achieved a weight loss of 10% or more. The study also found that bariatric surgery was associated with significant improvements in type 2 diabetes, high blood pressure, and sleep apnea.
- A systematic review and meta-analysis published in JAMA in 2018 found that bariatric surgery was associated with greater weight loss and improvements in type 2 diabetes, high blood pressure, and sleep apnea compared to non-surgical treatments such as medication and lifestyle interventions.
- A study published in Obesity Surgery in 2017 found that bariatric surgery was associated with significant improvements in mental health outcomes such as depression and anxiety.
- A study published in the New England Journal of Medicine in 2014 found that bariatric surgery was associated with a lower incidence of cardiovascular events such as heart attack and stroke compared to non-surgical treatments for obesity.
- A systematic review and meta-analysis published in the International Journal of Obesity in 2016 found that bariatric surgery was associated with greater weight loss and improvements in obesity-related health conditions compared to non-surgical treatments for obesity.
- A study published in Diabetes Care in 2016 found that bariatric surgery was associated with greater improvements in glycemic control (blood sugar levels) and diabetes remission compared to non-surgical treatments for obesity.
- A systematic review and meta-analysis published in Obesity Reviews in 2017 found that bariatric surgery was associated with greater weight loss and improvements in type 2 diabetes, high blood pressure, and sleep apnea compared to non-surgical treatments for obesity.
What Are the Risks of Bariatric Surgery?
Bariatric surgery is a major surgical intervention and carries risks and potential complications, as with any surgical procedure. Some of the potential risks and complications of bariatric surgery include:
- Bleeding: The surgical incisions made during bariatric surgery can sometimes result in bleeding, which may require additional surgery or blood transfusions.
- Infection: There is a risk of infection with any surgical procedure, and bariatric surgery is no exception. Infections can occur at the surgical site, in the lungs, or in the urinary tract.
- Blood clots: Surgery can increase the risk of blood clots forming in the legs, which can travel to the lungs and cause a pulmonary embolism.
- Bowel obstruction: Bariatric surgery can cause scarring or adhesions in the intestines, which can lead to a bowel obstruction.
- Dumping syndrome: This occurs when food moves too quickly through the stomach and intestines after surgery, causing symptoms such as nausea, vomiting, diarrhea, and dizziness.
- Nutritional deficiencies: Bariatric surgery can affect the body’s ability to absorb nutrients, leading to deficiencies in vitamins and minerals such as iron, calcium, and vitamin B12.
- Gallstones: Rapid weight loss after bariatric surgery can increase the risk of developing gallstones.
- Hernias: Surgery can increase the risk of developing hernias at the surgical site.
It’s important to note that these risks and complications are relatively rare, and most people who undergo bariatric surgery do not experience them.
However, it’s important to discuss the potential risks and benefits of bariatric surgery with a qualified healthcare provider before making a decision to undergo the procedure.
Alternative Obesity Treatment Methods
There are several alternative treatment methods for obesity that can be effective for some people. Here are some of the best alternative treatment methods:
Diet and exercise: A healthy diet and regular exercise can help promote weight loss and improve overall health. Eating a balanced diet that is rich in fruits, vegetables, lean proteins, and whole grains, and engaging in regular physical activity, such as brisk walking, cycling, or swimming, can be an effective way to manage weight.
Behavioral therapy: Behavioral therapy can help individuals identify and change negative behaviors and habits that contribute to obesity, such as overeating or emotional eating. Techniques such as cognitive-behavioral therapy (CBT) and mindfulness-based therapy can be effective for weight loss and weight management.
Prescription medications: Certain prescription medications, such as orlistat, lorcaserin, and phentermine/topiramate, have been approved by the FDA for the treatment of obesity. These medications work by reducing appetite, increasing feelings of fullness, or reducing the absorption of fat in the digestive system.
Medical weight loss programs: Medical weight loss programs, such as those offered by hospitals or weight loss clinics, can provide personalized weight loss plans and support from healthcare professionals.
Herbal remedies: Some herbal remedies, such as green tea, caffeine, and garcinia cambogia, have been suggested as potential aids for weight loss.
Let’s take a closer look at this last point, i.e. herbal treatments.
There are serious scientific studies on this, some of which are not very large, but shed some light on the subject.
But some of them provide sufficient infmation on the effectiveness of some herbal remedies.
While some people use herbal remedies for weight loss, the safety and effectiveness of these remedies are not well-established.
Some herbs that have been traditionally used for weight loss include green tea, Garcinia cambogia, and bitter orange.
Here’s what the research says about these herbal remedies:
- Green tea: Several studies have investigated the effects of green tea and its active compounds, catechins, on weight loss. A meta-analysis of 14 randomized controlled trials found that green tea catechins significantly reduced body weight and body mass index (BMI) compared to placebo, but the effects were modest. Another meta-analysis of 11 studies found that green tea supplementation led to a significant reduction in body weight and waist circumference, but the effects were greater in studies with higher doses of catechins and longer durations of treatment. A more recent randomized controlled trial found that green tea supplementation combined with exercise resulted in greater weight loss and reductions in BMI and body fat percentage compared to exercise alone.
- Garcinia cambogia:
Several studies have investigated the effects of garcinia cambogia and its active compound, HCA, on weight loss. A meta-analysis of 12 randomized controlled trials found that garcinia cambogia supplementation led to significant reductions in body weight, BMI, and waist circumference compared to placebo, but the effects were small. Another meta-analysis of 9 studies found that garcinia cambogia supplementation led to modest reductions in body weight and BMI, but the effects were not statistically significant. - Caffeine: Several studies have investigated the effects of caffeine on weight loss.
A meta-analysis of 11 randomized controlled trials found that caffeine supplementation led to modest reductions in body weight, BMI, and waist circumference compared to placebo, but the effects were greater in studies with higher doses of caffeine and longer durations of treatment. Another meta-analysis of 21 studies found that caffeine intake was associated with modest reductions in body weight, BMI, and body fat percentage, but the effects were greater in studies with higher baseline BMI and longer durations of follow-up. However, caffeine may have potential side effects, such as anxiety, insomnia, and increased heart rate, and further research is needed to determine its long-term safety and effectiveness. - Bitter orange:
Bitter orange contains synephrine, which has been shown to increase metabolism and promote fat burning. However, bitter orange has also been associated with adverse effects such as increased heart rate and blood pressure. The safety and effectiveness of bitter orange for weight loss are not well-established. - Fenugreek: Fenugreek is a plant that has been used traditionally for medicinal purposes, and some studies have suggested that it may have potential effects on blood sugar control and appetite regulation. A meta-analysis of 12 randomized controlled trials found that fenugreek supplementation led to significant reductions in fasting blood glucose levels and improvements in insulin sensitivity compared to placebo, but the effects on body weight and BMI were not statistically significant.
- Hoodia:
Hoodia is a cactus-like plant that has been used traditionally in South Africa to suppress appetite during long hunting trips. Some studies have suggested that hoodia supplementation may lead to reductions in calorie intake and appetite, but the effects may be small and further research is needed to determine its safety and effectiveness. - Turmeric:
Turmeric is a spice that contains curcumin, which has been investigated for its potential effects on inflammation and metabolism. Some studies have suggested that curcumin supplementation may lead to modest reductions in body weight and BMI, as well as improvements in lipid profiles and inflammation. However, the effects may be small, and further research is needed to determine optimal doses and durations of treatment. - Cinnamon:
Some studies have suggested that cinnamon may have potential effects on blood sugar levels and insulin sensitivity, which could indirectly affect weight loss. A meta-analysis of 10 randomized controlled trials found that cinnamon supplementation led to significant reductions in fasting blood glucose levels and improvements in insulin sensitivity compared to placebo, but the effects on body weight and BMI were also not statistically significant. - Konjac root:
Konjac root, also known as glucomannan, is a type of soluble fiber that has been investigated for its potential effects on weight loss and appetite control. Several studies have suggested that konjac root supplementation can lead to modest reductions in body weight and BMI, as well as improvements in satiety and food intake. However, the effects may be small, and further research is needed to determine optimal doses and durations of treatment. - Ginger:
Some studies have suggested that ginger may have potential effects on appetite control and calorie intake. A meta-analysis of 14 randomized controlled trials found that ginger supplementation led to significant reductions in body weight, BMI, and waist circumference compared to placebo, but the effects were modest.
Intensive Behavioral Therapy For Obesity
Intensive behavioral therapy is an effective treatment for obesity that focuses on helping individuals modify their eating and exercise habits.
By addressing poor habits that contribute to obesity, such as unhealthy eating patterns and a lack of physical activity, this therapy aims to facilitate weight loss.
During intensive behavioral therapy, you will work closely with a therapist either individually or as part of a group or using some apps (such as NOOM) that provide support in making lifestyle changes in order to succeed with permanent weight loss. These changes may include:
- Tracking your eating habits to become more aware of what and how much you consume.
- Modifying your environment to avoid situations that lead to overeating.
- Increasing your physical activity levels to burn calories and improve overall fitness.
- Developing an exercise plan tailored to your abilities and preferences.
- Setting realistic goals to ensure steady progress and maintain motivation.
By implementing these changes, you can expect to lose a significant amount of weight. Moreover, the skills and strategies learned during therapy can help you sustain your weight loss in the long term.
Why would I need intensive behavioral therapy for obesity?
Intensive behavioral therapy is an effective way to lose weight and maintain it. This therapy focuses on modifying your eating and exercise habits, aiding you in achieving lasting weight loss results.
By actively participating in this therapy, you can make positive changes to your behaviors and habits, leading to weight loss and improved overall health.
Moreover, by addressing obesity through behavioral therapy, you can reduce the risk of developing complications associated with conditions like diabetes over the long run.
The Results Of Intensive Behavioral Therapy For Obesity?
Intensive behavioral therapy is a long-term method that often spans several months. Even after reaching your desired weight, it can still be that you feel the need of guidance and support.
This could happen if you start regaining weight. By getting support, you can receive insights and strategies to overcome obstacles.
These resources can provide assistance in breaking through weight loss obstacles and maintaining your progress. One of these resources is Noom.
Imagine a world where achieving successful weight loss doesn’t require adhering to a restrictive diet.
Instead, it revolves around a psychology-based mobile app that transforms your daily behaviors. Enter Noom, a revolutionary app that dares to make this claim.
What Is Noom?
Noom is a mobile health app subscription service that goes beyond traditional diets. Since its inception in 2008 as a simple fitness and calorie tracker, Noom has evolved into a comprehensive program that incorporates psychology, behavioral change, and unwavering support.
What sets Noom apart is its team of esteemed behavioral health experts, dedicated to uncovering the underlying causes of weight loss struggles.
Extensive research in areas such as oncology, diabetes prevention, and hypertension has shaped Noom’s unique curriculum, focusing on the power of mindset before addressing meals.
Embark on a transformative weight loss journey with Noom’s holistic approach. It delves into your eating behaviors, helps you navigate emotional connections with food, instills a sense of accountability, and empowers you to make lasting lifestyle changes.
Noom isn’t just about shedding pounds temporarily—it’s about achieving sustained weight loss and embracing a healthier lifestyle for the long run.
How Does Noom Work?
[As we mentioned earlier, we are not an affiliate partner with Noom. Not all of the products we recommend bring us revenue and we do not recommend any product to generate revenue if we do not believe in the effectiveness of the product.] The Noom diet plan takes a unique approach by asking thought-provoking questions that you may not have encountered with other diet plans.
- Begin with a personalized plan through an interactive quiz.
The first step of the Noom program involves taking a brief 10-minute online quiz. This quiz asks you common questions about your height, weight, gender, age, and your reasons for wanting to lose weight. It also gathers information about your activity level, eating habits, and any potential health concerns such as diabetes, heart disease, or depression. In addition, it delves into aspects like life events that may have contributed to weight gain and explores any uncertainties you may have about achieving your weight loss goals.
- Sign up and access the app on your smartphone.
After making the decision to join the program and completing the payment, you can easily download the Noom app on your smartphone. The app is currently available for both IOS (version 12.4 or later) and Android (version 6 or later) devices. While it can also be used on tablets, please note that the functionality may be limited as tablets typically lack motion sensors, which are used for features like the step counter. Once the app is installed, you’ll be prompted to sign in using the email address you provided during the sign-up process.
- Engage with your coaches, embrace the lessons, and receive your calorie budget.
Noom introduces you to the world of psychology and behavioral change through 10 comprehensive mini-lessons to be completed within a 16-week period.
You have the flexibility to decide how much time you want to dedicate each day to these lessons, with a minimum of five minutes and a maximum of 16 minutes.
Around two days into the program, you will be connected with a dedicated goal coach who will check in with you twice a week, providing support, tracking your progress, and offering motivational messages.
As you progress further, you will also be assigned a group coach and be placed in a peer group. The group coach plays a crucial role in moderating the peer group chat, sharing weight loss tips, and occasionally responding to individual posts.
Both the goal coach and group coach possess extensive knowledge of Noom and have received proper training, holding either a bachelor’s or associate’s degree along with 2,000 hours of wellness experience.
Noom tailors your calorie restrictions specifically to your personal information. In certain cases, if you are obese or pre-diabetic, Noom may recommend its diabetes prevention program.
Notably, this program holds the distinction of being the first mobile health program recognized by the Centers for Disease Control (CDC) for its effective delivery of an evidence-based type 2 diabetes prevention program.
With your personalized plan from Noom, you will be assigned a daily calorie budget tailored to your needs. This budget represents the minimum calories required for your body to function optimally each day.
You will be prompted to record your meals and physical activity on a daily basis. Additionally, you have the flexibility to allocate two to 10 minutes per day for reading short articles on positive thinking, mindful eating, and stress relief.
Noom goes the extra mile by providing a step counter feature. As long as your phone is with you throughout the day, you will have access to valuable insights on your total number of steps taken.
The app also encourages you to log other important health metrics such as blood pressure readings, blood glucose levels, and water intake.
The Noom plan is designed to span over 16 weeks, but you have the option to purchase up to twelve months at a time for both weight loss and maintenance purposes.
As an example, if your goal is to lose 12 pounds, your calorie budget may be set at 1,250 calories per day for the duration of the 16-week plan.
When logging your foods, the app will inform you of the remaining calories available within each food category for the day. Importantly, there is no admonishment if you happen to exceed your calorie budget.
Instead, Noom provides encouraging messages to keep you motivated and offers lessons to help you reflect on the triggers behind any unhealthy eating episodes you may have experienced.
Foods You Can Eat With Noom
Noom stands out from other plans I’ve tried because it doesn’t restrict any specific foods or food groups. Any limitations are up to you. While Noom offers options for vegan, gluten-free, or low-carb diets, it never categorizes foods as “bad” or off-limits.
At Noom, they believe that the weight of food, not just the number of calories, affects how satisfied you feel. To address this, they use a color-coded food system based on caloric density (CD).
Foods with higher water content and lower CD are considered more favorable because they can make you feel fuller with fewer calories.
Here’s how the color-coded system works:
- Green Foods: This category includes fruits, vegetables, and whole grains. These foods have a low caloric density, meaning they are high in water content and rich in nutrients. They should make up a significant portion of your diet.
- Yellow Foods: Lean meats, legumes, and low-fat dairy fall into this category. They have slightly higher calories and fewer nutrients compared to green foods. It’s advised to consume them in moderation.
- Red Foods: This category includes red meats, processed foods, and full-fat cheese. These foods have the highest caloric density and provide fewer healthy nutrients.
As per the information provided on the Noom website, here is a breakdown of food examples for each color category
Green:
- Vegetables: tomatoes, cucumbers, salad greens, carrots, onions, spinach
- Fruits: bananas, apples, strawberries, watermelon, blueberries
- Starchy vegetables: parsnips, beets, sweet potatoes, squash
- Dairy: skim milk, nonfat yogurt, nonfat Greek yogurt, nonfat cheese sticks
- Whole grains: oatmeal, brown rice, whole grain bread, whole grain pita, whole grain pasta, whole grain tortilla, whole grain cereals
- Dairy alternatives: unsweetened almond, cashew, or soy milk
- Condiments: marinara, salsa, sauerkraut, ketchup, light mayo
- Beverages: unsweetened tea and coffee
Yellow:
- Lean meats: grilled chicken, turkey, and lean cuts of beef, pork, and lamb
- Legumes and seeds: lentils, pinto beans, chickpeas, peas, quinoa, black beans, soybeans
- Seafood: tuna, salmon, tilapia, scallops
- Grains and grain products: couscous, white rice, white bread, white pasta
- Dairy: low-fat milk, low-fat cheeses, low-fat cottage cheese, Greek yogurt
- Beverages: diet soda, beer
Orange (previously red):
- Nuts and nut butters: peanut butter, almond butter, almonds, walnuts
- Meats: ham, red meats, fried meats, bacon, sausage, hot dogs, hamburgers
- Condiments and toppings: butter, mayonnaise, ranch dressing
- Snack foods: french fries, potato chips, energy and snack bars
- Desserts and sweets: cake, chocolate, cookies, candy, pastries
- Beverages: wine, juices such as orange juice
Noom suggests consuming them in smaller portions, typically making up around 25% of your daily calorie intake.
Noom never prohibits you from having “red” foods. Instead, it encourages mindfulness about your consumption.
Every time you log a food, Noom automatically classifies it with a color, allowing you to visually assess areas where your diet may need improvement.
By following the Noom system, you can discover that it’s possible to achieve significant weight loss while enjoying a wide range of foods.
What Does Noom Cost?
Noom offers a free one-week trial for users to experience their program before making a commitment.
If you choose to continue, subscription prices for their individualized plans start at $59 per month.
The duration of the program will vary depending on your weight loss goals.
Noom offers a range of subscription plans with varying durations and prices:
- Monthly auto-renewing plan: $70 per month
- 2-month auto-renewing plan: $129 (equivalent to $64.50 per month)
- 3-month auto-renewing plan: $159 (equivalent to $53 per month)
- 4-month auto-renewing plan: $169 (equivalent to $42.25 per month)
- 5-month auto-renewing plan: $174 (equivalent to $34.80 per month)
- 6-month auto-renewing plan: $179 (equivalent to $29.83 per month)
- 7-month auto-renewing plan: $184 (equivalent to $26.29 per month)
- 8-month auto-renewing plan: $189 (equivalent to $23.63 per month)
- 9-month auto-renewing plan: $195 (equivalent to $21.67 per month)
- 10-month auto-renewing plan: $199 (equivalent to $19.90 per month)
- 11-month auto-renewing plan: $205 (equivalent to $18.64 per month)
- Annual auto-renewing plan: $209 (equivalent to $17.42 per month)
Noom’s pricing may surpass what you are willing or able to invest, but it is widely regarded as one of the most effective programs for overweight individuals seeking a sustainable and straightforward approach to weight loss.
Pros and Cons of Noom
Pros of Noom
- Utilizes a simple color-coded system to promote foods with a low calorie density.
- Does not restrict or eliminate any specific foods or food groups, allowing for flexibility and personalization.
- Focuses on behavioral changes to foster sustainable lifestyle habits.
- Provides support from a virtual coaching team, offering guidance, motivation, and accountability.
- Allows users to easily adjust their goals to fit their individual needs and preferences.
- Offers educational resources, quizzes, and challenges to help users understand and address the psychological factors influencing their eating habits.
- Incorporates biometric tracking features to monitor blood sugar and blood pressure levels for improved health management.
- Provides tools to track progress, including logging meals, exercise regimens, and body weight.
- Offers a 7-day trial period to allow users to experience the app before committing to a subscription.
- Can be accessed through a mobile app, making it convenient for users to track their progress on-the-go.
Cons Of Noom
- Relatively higher price point compared to other options available.
- Places greater emphasis on achieving weight loss rather than overall holistic well-being.
- Solely provides virtual coaching as a means of support.
- Requires the use of a smartphone or tablet for access.
- Categorizes several nutrient-rich foods as “orange” within its system.
- Recommends a lower calorie intake, which may not be suitable for everyone’s needs.
- Involves the potentially time-consuming task of logging and tracking food consumption.
Accountability & Support
Noom promotes accountability by encouraging you to not only consider the food you consume but also the underlying thoughts guiding your choices. Certified health coaches provide weekly check-ins to offer encouragement. The app also facilitates connections with fellow Noomers.
How Much Weight Can You Lose On Noom?
Noom suggests that maintaining a consistent calorie intake towards the lower end of your Weight Loss Zone, which represents the necessary range, can result in an average weight loss of approximately two pounds per week.
Conversely, adhering to the higher end of your Weight Loss Zone may lead to an average weight loss of about half a pound per week, according to Noom’s guidelines.
Does Noom Work for Vegans & Vegetarians?
Noom assures that its weight loss plan is suitable for vegetarians, vegans, and other plant-based diets.
The program includes plant-based recipes as part of its premium features, and Noom’s coaches are ready to assist subscribers in transitioning to a more plant-forward diet, if desired.
Noom offers a valuable premium feature, which is a recipe database sourced from Rodale, Inc., a famous publisher of health websites such as Prevention, Women’s Health, and Men’s Health.
With over 1,100 recipes available, the database is conveniently organized into categories including breakfast, lunch, dinner, and snacks.
Long-Term Results From 36000 Participants Using Noom
Research examining long-term weight loss studies indicates that, on average, people regain 33% of their initial weight loss after 1 year and 79% after 5 years.
Recognizing the challenges associated with behavioral change, Noom implements a psychology-based curriculum.
By focusing on these psychological factors, Noom aims to provide individuals with the tools and knowledge needed to make sustainable behavioral changes, essential for long-term weight management.
Notably, a study involving nearly 36,000 Noom users demonstrated that 78% were able to sustain their weight loss over a period of 9 months.
Frequently Asked Questions On Being Overweight
What Is A Healthy Waist For A Man?
For men, a waist circumference below 94cm (37in) is considered ‘low risk’, while 94–102cm (37-40in) falls under the ‘high risk’ category, and anything above 102cm (40in) is labeled as ‘very high risk’.
As for women, a waist measurement below 80cm (31.5in) is considered ‘low risk’, while 80–88cm (31.5-34.6in) is categorized as ‘high risk’, and any measurement above 88cm (34.6in) is labeled as ‘very high risk’.
Monitoring waist circumference is vital for assessing health risks associated with weight and obesity.
How Much Weight Do You Need To Lose To Fix ED?
An Australian study, featured in the “Journal of Sexual Medicine,” revealed that shedding as little as 5% to 10% of body weight in a span of two months led to notable improvements in erectile function and heightened sex drives for obese men with diabetes.
Additionally, a separate research conducted at a renowned medical institute demonstrated similar positive outcomes, emphasizing the crucial role of weight loss in enhancing sexual health among men with obesity-related conditions.
Furthermore, a follow-up study at a leading university corroborated these findings, indicating that moderate weight reduction can have a significant impact on erectile function and overall sexual well-being in this particular group of patients.
Does Losing Weight Increase blood Flow?
Losing weight can increase blood flow, particularly in individuals who are overweight or obese. Excess body weight, especially around the abdominal area, is associated with the accumulation of fatty deposits in blood vessels, which can restrict blood flow. By losing weight, the burden on the circulatory system is reduced, leading to improved blood flow throughout the body, including to the genital region.
There are studies that support the relationship between weight loss and increased blood flow:
-
A study published in the “Journal of the American College of Cardiology” in 2013 investigated the effects of weight loss on vascular function in overweight and obese individuals. The results demonstrated that a moderate weight loss of approximately 7-10% improved endothelial function, which is a measure of blood vessel health and dilation, leading to enhanced blood flow.
-
Another study published in the “Journal of Sexual Medicine” in 2017 examined the effects of weight loss on erectile function in obese men with diabetes. After losing 5% to 10% of their body weight over a two-month period, the participants experienced significant improvements in erectile function, which were attributed to enhanced blood flow to the penile region.
These studies provide evidence that weight loss can positively impact blood flow and, in turn, improve various aspects of health, including vascular function and erectile function. However, it’s essential to remember that individual responses to weight loss may vary.
What Causes Belly Fat In Males?
Belly fat, also known as visceral fat, can accumulate in males due to a combination of various factors, including:
-
Poor Diet: Consuming a diet high in calories, unhealthy fats, added sugars, and processed foods can contribute to excess belly fat. Frequent intake of sugary beverages, refined carbohydrates, and unhealthy snacks can lead to weight gain, particularly in the abdominal area.
-
Sedentary Lifestyle: Lack of physical activity and a sedentary lifestyle can lead to the accumulation of belly fat. When energy intake exceeds energy expenditure, the body stores excess calories as fat, and the abdominal region is a common site for fat storage.
-
Genetics: Genetic factors can play a role in determining the distribution of fat in the body, including around the belly. Some individuals may be genetically predisposed to storing fat in the abdominal area.
-
Hormonal Changes: Hormonal imbalances, such as elevated cortisol levels due to chronic stress, can contribute to the accumulation of belly fat. Cortisol is a stress hormone that, when elevated over time, can lead to fat storage, particularly in the abdominal region.
-
Age: As men age, their metabolism tends to slow down, and they may experience a decrease in muscle mass. These changes can lead to an increase in body fat, especially around the belly.
-
Alcohol Consumption: Excessive alcohol intake can contribute to weight gain, including the accumulation of belly fat.
-
Medical Conditions: Certain medical conditions, such as insulin resistance, polycystic ovary syndrome (PCOS), and hormonal imbalances, can contribute to the development of belly fat in males.


